Eye-popping predictions for weight-loss drug sales hinge on insurance companies agreeing to provide coverage for expensive treatments, and momentum appears to be building on that front. But Allen Lutz, an analyst at Bank of America, wonders if employers know how risky the bet they’re making is. The hope is that current spending on GLP-1 drugs such as Ozempic, which can cost $1,300 a month or more, will result in health care savings tomorrow. “We question whether employers adding coverage to GLP-1s in 2024 fully appreciate both the off-label use of the drug (which occurs outside the scope of benefits) and the potential for increased adherence ” Lutz wrote in a research note Monday. . Lutz’s comments follow a survey showing that the number of employers planning to provide insurance coverage for these drugs is expected to nearly double. The survey was conducted by market researcher Savanta on behalf of Accolade, a healthcare benefits navigation service provider, and surveyed 500 human resources managers in August and September. In the survey, 43% said they plan to offer GLP-1 coverage in 2024, an increase from the 25% of employers who currently offer it. Accolade also said 81% of HR representatives believed employees would be interested in having access to the medications. GLP-1 drugs were first approved to treat type 2 diabetes, but are now used to treat obesity and being overweight. The drugs include Novo Nordisk’s semaglutide, sold as Ozempic for diabetes management and as Wegovy for weight loss. Eli Lilly makes Mounjaro, also known as tirzepatide. It received approval from the U.S. Food and Drug Administration last year to treat type 2 diabetes and could gain approval for obesity by the end of this year. Both medications can help patients lose 15% or more of their initial weight. Unlike previous generations of weight loss drugs, their side effects were largely mild and included diarrhea, constipation and nausea. Wegovy’s label also includes warnings about pancreatitis and certain types of intestinal obstruction. Although designed to treat overweight and obesity, the drug has been used off-label by people who wanted to lose weight for cosmetic reasons, which is a concern raised by Lutz. “Moreover, employers continue to wonder how to encourage patients to make long-term lifestyle and behavior changes to support permanent weight loss, consider potential long-term side effects, while managing higher costs associated with coverage,” says the health services industry. said the analyst. Higher hospital labor costs as well as GLP-1 drugs are contributing to the largest increase in health insurance costs since 2012, Lutz said. He cited a recent estimate from consulting firms Mercer and Willis Towers Watson that predict a 6.5% increase in insurance costs between 2023 and 2024. Insurers are already feeling the effects even though these drugs are still in their infancy. ‘in their beginnings. In a research note Wednesday, Citi analyst Peter Verdult estimated that GLP-1 sales could reach $30 billion for diabetes and $6 billion for obesity this year. “Penetration remains modest,” Verdult said. He expects that fewer than 10 percent of diabetic patients will take these medications and fewer than a million obese patients will be treated. But those numbers will rise, especially as ongoing research continues to demonstrate benefits beyond blood sugar control and weight loss. For example, the drugs have shown cardiovascular benefits as well as potential kidney and liver benefits. Novo Nordisk and Eli Lilly are also examining whether GLP-1 drugs could help people with alcohol dependence, sleep apnea and other conditions. More than 40% of American adults suffer from obesity, according to the Centers for Disease Control and Prevention. Taking into account overweight people increases the potential population of this drug to more than 70% of adults. Doctors consider obesity a chronic disease. Many patients who have successfully lost weight with a GLP-1 medication find that they regained weight after stopping taking it. This has prompted some analysts to predict that these drugs will see peak sales of more than $100 billion, as they become as widely prescribed as cholesterol-lowering statins. CNBC’s Michael Bloom contributed to this report.
#Bank #America #Sees #Risks #Employers #Insurance #Coverage #Weight #Loss #Drugs #Increases
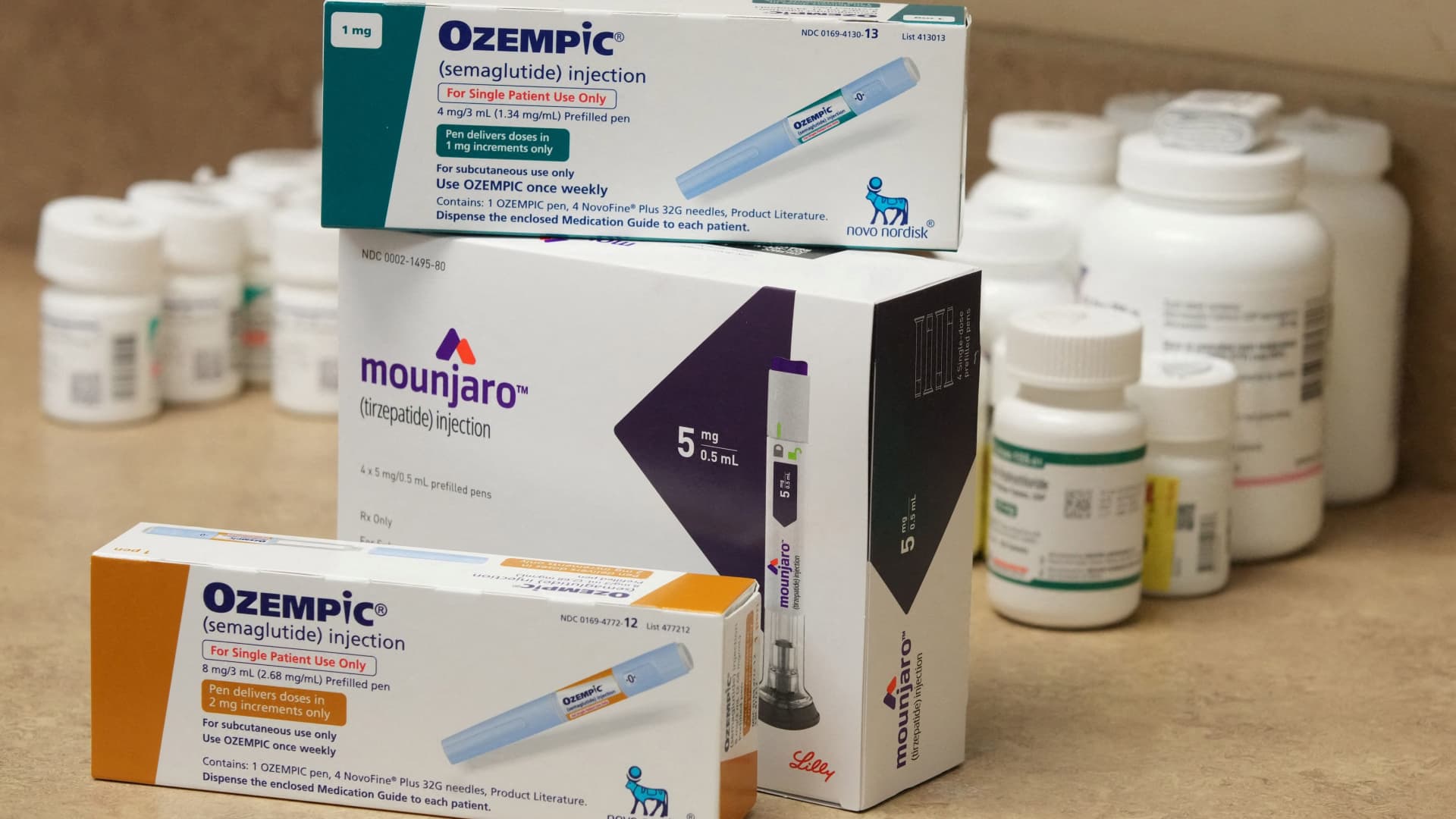
Image Source : www.cnbc.com